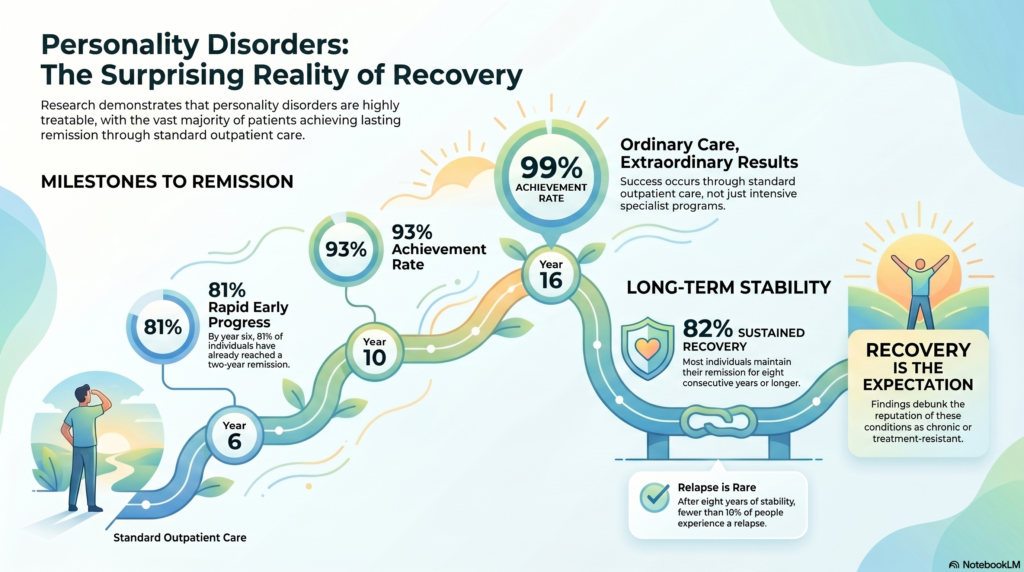
Recovery is the Most Likely Outcome
For many people, a diagnosis like borderline personality disorder (BPD) can feel overwhelming or even make them feel broken. Today, we’re exploring the traditional 10 personality disorders and the new model that’s changing how we understand ourselves (and our loved ones). But first, a dose of hope: the reality is that most people who seek recovery for personality disorder traits achieve remission, meaning they no longer meet diagnostic criteria.
5 Traits > 10 Disorders?
Personality disorders have traditionally been diagnosed and discussed as fixed conditions, as though they are something a person is, rather than something they are experiencing. But as the remission and recovery data show us, disordered personality traits are highly mutable.
As such, diagnosis is shifting from the categorical and binary approach to a more fluid dimensional model, viewing personality disorders more as patterns of thinking, feeling, and relating to the world that have become rigid or exaggerated enough to cause difficulty in everyday life.

At CooperRiis, we have always taken a nuanced, spectrum-oriented approach to treating personality disorders. We focus on the whole person and those parts of the person that transcend diagnosis. In this paradigm, residents heal patterns, and important pathways towards change emerge, because patterns can and do change. Diagnosis is often important, but we have always avoided focusing on labels that are unhelpful or unnecessarily limiting.
What is a Personality Disorder?
At their core, personality disorders are maladaptive patterns in the way a person tends to experience themselves, relate to others, and respond to stress. These patterns can show up in emotions, beliefs, relationships, and behaviors.
Most of the traits that characterize personality disorders, even the maladaptive ones, exist in all of us to one degree or another. The question isn’t whether a trait is present, but rather:
- How intense is this trait?
- How much inflexibility has grown up around it?
- Is this trait interfering with daily life and relationships?

A pattern can become a disorder when it stops helping us to adapt and cope with life’s ups and downs and instead starts getting in the way of relationships, work, stability, and quality of life.
While our clinicians carefully consider diagnosis and may use traditional diagnostic language as a tool for communicating with patients and their families, diagnosis is not the focus of our work. Used carefully, a personality disorder diagnosis doesn’t need to feel like a defining label and can actually help a person and their family to understand what’s happening, access the right kind of support, and feel hopeful about the future.
What Are the 10 Personality Disorders?
For decades, clinicians have relied upon a system that organizes 10 clinically recognized personality disorders into three clusters that share certain thematic traits. But clinical descriptions can take us only so far. What does it really feel like to live with a personality disorder? The brief first person summaries below offer a glimpse into how each it may feel in everyday life.
Cluster A: “Odd” or Distant Patterns
Cluster A often reflects a mix of withdrawal, guardedness, and difficulty feeling safe or at ease with others, sometimes combined with mistrust or unusual thinking. People may appear cold, suspicious, or eccentric, but are often trying to protect themselves from feeling hurt, overwhelmed, or misunderstood.

- Paranoid personality disorder: I often feel that others may be deceptive or untrustworthy. I see threats or hidden motives that others don’t see, and it’s difficult for me to let go of slights. People may say they’re on my team, but I have a hard time believing that anyone has only my best interests at heart.
- Schizoid personality disorder: I feel most comfortable on my own and prefer to keep others at a distance. People often expect me to express more emotion or engage more in relationships, but being alone feels easier and more natural to me.
- Schizotypal personality disorder: I often feel out of step with others and anxious or self-conscious in social situations. Sometimes what I say or do doesn’t seem to come across the way I intend, and I’ve gotten used to feeling like the odd one out.
Cluster B: Intense, Emotional, and Relational Patterns
Cluster B is often associated with intensity in identity, relationships, and emotional experience. People in this cluster may carry deep sensitivity, pain, fear, or shame, and may struggle with closeness, trust, or a stable sense of self. In relationships, emotions can escalate quickly, interactions feel high-stakes, and reactions are often unpredictable.

- Antisocial personality disorder: Rules feel more like suggestions to me, especially if they get in the way of what I need. If I cut corners or bend the truth, I generally focus more on whether I’ll get caught than on how it affects others.
- Borderline personality disorder: I care deeply about the people in my life, but that intensity sometimes feels overwhelming. Seemingly small moments, like someone I care about not calling me back right away, can cause me to quickly go from feeling loved to feeling abandoned.
- Histrionic personality disorder: I feel most alive when I have others’ attention. I often move quickly into close relationships, but I can get anxious if I sense someone pulling away, and I may try to reconnect in ways others don’t understand.
- Narcissistic personality disorder: People see me as very self-confident, but underneath, I feel very sensitive to criticism or being overlooked. When I feel exposed, I feel a strong need to protect myself, even if it causes strain in my relationships.

Cluster C: Anxious and Controlling Patterns
The patterns in Cluster C are often shaped by fear, insecurity, sensitivity to evaluation or rejection, and difficulty tolerating uncertainty. There is often a strong desire to stay safe and avoid mistakes, sometimes at the expense of flexibility, independence, or connection.
- Avoidant personality disorder: I want close relationships more than it may seem, but my fear of being judged or rejected holds me back. Compliments can be hard to take in, while criticism tends to stay with me and feels like a confirmation of my worst fears.
- Dependent personality disorder: I often feel unsure of myself when I have to make decisions on my own. Without someone’s decisive support or reassurance that I’m doing the right thing, I might second-guess myself so much that even small decisions feel overwhelming.
- Obsessive-compulsive personality disorder (OCPD): I often find myself very focused on doing things the “right” way. Details matter to me more than they seem to matter to others. I’m not trying to be controlling, but predictable structure helps me to feel safe.
Why the Cluster Model Works
The conventional system for diagnosing the 10 personality disorders has long been this categorical approach: either you meet criteria for a disorder, or you don’t.
That simplicity has real benefits:
- It gives people a name for what they’re experiencing.
- It aids clinicians in communicating clearly with patients and among themselves.
- It makes clinical research easier to conduct and organize.
For many patients and their families, receiving a diagnosis can be a relief. They finally have a name for what they’ve been experiencing, and they know they’re not alone. But categorical diagnosis doesn’t tell the whole story of who a person is and what they’re capable of. Furthermore, every patient (and each of their family members) relates to diagnosis differently. Consumer opinion on the diagnostic systems varies: some find labels helpful, while others find them limiting.
The Trouble with Clusters
Real people don’t fit neatly into categorical boxes, and some issues with the binary diagnostic model have become apparent over time:
- Overlap (comorbidity): Many people meet criteria for multiple disorders at different times in their lives.
- Arbitrary thresholds: Someone can be struggling significantly in daily life, but still not “qualify” for a disorder within the conventional model.
- Heterogeneity: Two people with the same diagnosis may behave completely differently.
These difficulties can affect how people are understood, how they view healing, and their orientation to the future, all of which may present real barriers to accessing treatment.
The DSM-5 Alternative Model of Personality Disorders
A new way of thinking is slowly emerging from research into practice. Instead of asking: “Which disorder does this person have?” The alternative, or dimensional, model asks: “What patterns are present, and how severe are they?” This approach, outlined in the DSM-5 alternative model, shifts the focus to an empirically based approach to classifying personality that measures a person’s level of impairment and their underlying personality traits.
In plain language, the DSM-5 and the broader mental health community are coming around to what we at CooperRiis have always believed: that personality traits exist on a spectrum, and that those traits can and do change with time, circumstances, and the right supports.
The Five Personality Trait Domains
The dimensional model organizes personality patterns into five broad trait types that map more closely with real human variation and allow clinicians to describe a person’s experience with more precision. The dimensional model measures the extent to which these five broad trait types, which exist to some degree in all of us, are present and whether they are impairing relationships or diminishing quality of life.

- Negative Affectivity includes difficult emotions such as anxiety, shame, anger, and reactivity.
- Detachment describes social and emotional withdrawal or reduced desire for closeness and connection.
- Antagonism includes grandiosity, hostility, low empathy, and deceitfulness.
- Disinhibition refers to difficulty with impulsivity and self-control.
- Psychoticism is characterized by unusual thinking, perceptions, or beliefs and eccentricity.
Why The Dimensional Model Works
This shift can change how patients and families understand their experience and improve how care is provided. It’s a more personalized approach with valid clinical utility because it:
- Captures people who fall through the cracks: Those who don’t meet the full criteria for a single disorder, but may still be struggling, are no longer invisible and untreated or undertreated.
- Reflects real complexity: Someone can be highly emotionally reactive, somewhat avoidant, and mildly impulsive. A single label can’t capture that, but a trait profile can.
- Improves treatment planning: Research suggests that a nuanced understanding of trait patterns can improve communication, planning, and monitoring.
Traits Can Change
The Collaborative Longitudinal Personality Disorders Study found that personality disorders are not as fixed as we once believed, and maladaptive traits often improve significantly over time, especially with thoughtful and careful treatment. This is where the dimensional model becomes especially powerful. Instead of saying: “The diagnosis is still there.” We can identify when specific patterns and traits are improving, along with patient satisfaction and quality of life.
A Both/And Approach
The future is likely a hybrid of both categories and dimensions, allowing us to access the best each approach has to offer. Traditional categories and diagnosis can help us name and communicate patterns more clearly and effectively, and a dimensional understanding can help us to understand and treat them more precisely, offering hope for change at the outset.
Used together, both approaches offer us something better than either one can alone: a clear, clinically supported understanding that growth and change are natural responses to treatment, and that healing is possible.

A More Human Way of Understanding Personality
Personality disorders should not be viewed as character flaws or fixed identities, but rather as patterns shaped over time in response to our circumstances. For many people experiencing disordered personality traits, these patterns began as beneficial, adaptive coping strategies. It is when these traits become rigid that they begin to interfere with our quality of life and intimate relationships, but this is by no means permanent.
For someone living with a personality disorder, or families trying to understand a diagnosis, that distinction is significant. Suddenly the story shifts from: “This is who they are” to: “Growth and change are possible.” Now, there is space for:
- Patterns to shift
- Severity to decrease
- Functioning to improve
- Hope for the future to emerge
How CooperRiis Can Help
In a residential treatment setting, individuals have the space and support to expand their flexibility, restore agency, and build a stable life that feels their own. Care in CooperRiis’ programs is immersive, consistent, and grounded in real-life practice. The work we do centers on helping people notice patterns as they arise, understand what those patterns are trying to accomplish, and develop ways of responding that are more effective and more aligned with who they want to be.

Because of our focus on healing in community, and because residents are active participants in their own care, change rapidly translates to lived experience. Patterns that once felt automatic take a back seat as new responses become more accessible. Over time, people often find that the rigid traits which limited them can be softened and retooled into strengths.
In this way, mental health recovery is not about becoming someone different, but about creating the space to think clearly, choose intentionally, and connect.
Additional References
Morey, L., & Benson, K. (2016). Relating DSM-5 section II and section III personality disorder diagnostic classification systems to treatment planning. Comprehensive Psychiatry, 68, 97-105. https://doi.org/10.1016/j.comppsych.2016.03.010
Morey, L., Hopwood, C., Gunderson, J., Skodol, A., Shea, M., Yen, S., … & McGlashan, T. (2006). Comparison of alternative models for personality disorders. Psychological Medicine, 37(7), 983-994. https://doi.org/10.1017/S0033291706009482
Skodol, A. (2011). Revision of the personality disorder model for DSM-5. American Journal of Psychiatry, 168(1), 10-14. https://doi.org/10.1176/appi.ajp.2010.10101466