If you or a loved one has been diagnosed with bipolar disorder or a related condition, we want you to know:
There is hope.
Our holistic residential treatment programs for bipolar disorder have helped adults aged 18+ regulate their moods effectively, cultivate emotional stability, and regain control of their lives.
We can help you or your loved one too.
Recovery is Possible
Our Approach to Healing Bipolar Disorder
Authored by Eric Levine, Ed.D. and Reviewed by Amy Zimmerman, DO Psychiatrist
A Focus on Wellness & Possibility
Bipolar disorder can jumble people’s senses of self, fracture their relationships, and turn day-to-day life into a confusing tumult. That’s why we begin our bipolar residential treatment programs by helping individuals with this condition make sense of both it and themselves. At The Farm (our long term residential treatment center) and CooperRiis at Asheville (our short-term residential treatment center), we remove the stigma and shame associated with bipolar disorder, shifting residents’ focus from negative experiences they’ve had in the past towards uplifting possibilities we firmly believe they can achieve in the future.What is bipolar disorder?
Bipolar disorder is a mood disorder that affects 2.6 percent of American adults. It is characterized by extreme variability in temperament that includes periods of mania or hypomania and periods of depression. Individuals with this condition experience dramatic shifts in energy level, emotionality, self image, and connection to reality throughout their lives. These shifts make it very difficult to maintain work, relationships, and personal health over time.
What are the signs and symptoms of bipolar disorder?
Bipolar disorder is associated with a broad spectrum of symptoms that vary significantly in severity from person to person. The hallmark of this condition is the experience of dramatic changes in mood, energy, sleep, and behavior that are so severe, they threaten personal wellbeing and safety. For an individual to be diagnosed with bipolar disorder, they must have had at least one manic or hypomanic episode.
Manic Episodes:
During manic episodes, an individual experiences an elevated state — usually lasting about one week — in which they may:
- Have trouble sleeping or less need for sleep
- Excessive and irrational worry
- Feel restless
- Feel wired
- Feel elated
- Feel agitated or irritable
- Talk more than usual
- Talk loudly or rapidly
- Have trouble focusing
- Have increased activity levels, doing many activities at once, overscheduling
- Be more impulsive
- Engage in risky behaviors (e.g.: reckless sex, reckless driving, reckless spending)
- Have an unusually high sex drive
- Have uncontrollable, racing thoughts
- Experience disjointed thinking
- Have an exaggerated sense self-esteem or grandiosity
- Experience psychosis
- Engage in drug and/or alcohol abuse
Hypomanic Episodes:
Hypomanic episodes are less severe than manic episodes; they last at least four days in a row and are characterized by similar symptoms that are more moderate in intensity.
Depressive Episodes:
In addition to manic or hypomanic episodes, individuals with bipolar disorder also experience major depressive episodes. These typically last at least two weeks and feature at least five of the following symptoms, including one of the first two in the list:
- Intense sadness or despair; feeling helpless, hopeless, or worthless
- Loss of interest in activities once enjoyed
- Feeling guilty
- Feeling worried
- Feeling empty
- Becoming forgetful
- Experiencing changes in sleep patterns such as sleeping too little or too much
- Feeling restless or agitated
- Having slowed speech or moving slowly
- Eating too much or too little
- Experiencing energy loss, fatigue
- Having difficulty making decisions
- Having frequent thoughts of death or suicide
- Declining activity levels
- Experiencing difficulty concentrating
Mixed States:
Between manic/hypomanic and depressive episodes, individuals with bipolar disorder may also experience mixed states with symptoms of both the former and the latter at once. Examples include:
- Feeling energized and hopeless at the same time
- Feeling restlessness and emptiness together
Because such a wide range of symptoms are associated with bipolar disorder, it’s often mistaken for other conditions, such as borderline personality disorder (BPD) or schizophrenia. If you suspect that you or a loved one may be experiencing bipolar disorder, it’s important to schedule a full psychiatric evaluation with a professional who can provide an accurate diagnosis if necessary.
What are the four different types of bipolar disorder?
The four basic types of bipolar disorder are:
- Bipolar I disorder
- Bipolar II disorder
- Cyclothymic disorder
- Unspecified bipolar and related disorders
All four types involve changes in mood, energy, and activity levels that impede daily functioning, interrupt healthy relationship development, and can jeopardize personal safety.
Bipolar I Disorder:
To be diagnosed with bipolar I disorder, a person must have a manic episode that lasts at least seven days or have manic symptoms so severe that immediate hospitalization is required. Usually, an individual who meets this criteria has also experienced one or more depressive episodes, but that is not necessary for diagnosis. Between periods of mania and depression, individuals with bipolar I disorder can feel normal.
Bipolar II Disorder:
Individuals with bipolar II (vs. bipolar I) disorder do not enter states of full-blown mania. Instead, they experience depressive episodes — sometimes longer and more severe than those experienced by individuals with bipolar I disorder — interspersed with hypomanic episodes. Between periods of depression and hypomania, individuals with this condition can feel normal.
Cyclothymic Disorder:
Cyclothymic disorder is a milder form of bipolar disorder. Individuals with this condition experience a chronically unstable mood with alternating hypomania and depression symptoms for at least two years. Though these symptoms are less severe than the symptoms associated with bipolar I or bipolar II disorder, they impede day-to-day functioning.
Other Specified/ Unspecified:
Those who do not meet the diagnosis criteria for bipolar I, bipolar II, or cyclothymic disorder but still experience significant mood swings and/or mood elevation may receive a diagnosis of “other specified” or “unspecified” bipolar disorder.
Is bipolar disorder genetic?
Research is still being conducted on what causes bipolar disorder; scientists believe that a mixture of genetic and environmental factors can predispose individuals to developing this condition.
Can bipolar disorder go away?
There currently is no “cure” for bipolar disorder. However, with holistic, relationship-driven treatment and strong support networks, individuals with this diagnosis can learn how to manage their symptoms, regulate their moods, and live full, gratifying lives. If you want to learn more about whether residential treatment for bipolar disorder at CooperRiis is right for you or your loved one, give us a call today
Dream Statements
Education and Empowerment
Psychoeducation is a critical facet of recovery for individuals with bipolar disorder. That's why we not only conduct a comprehensive psychiatric evaluation for every resident that enters our care, but we also make sure to discuss evaluation results with residents themselves. We make sure that individuals who are diagnosed with bipolar disorder understand why and how this condition affects them.
Then, we work with each resident to develop a recovery plan that suits their needs and preferences. This plan involves lifestyle modifications that will keep their symptoms from flaring up. By helping residents with bipolar disorder choose career paths, create routines, and develop social habits that promote stability, we empower them to become stewards of their own health.
Relationship-Driven, Resident-Centered Care
The success of our approach to treating bipolar disorder hinges on the trusting relationships we cultivate with residents. We take the time to understand their preferences and thoroughly explain our recommendations as we partner with them to create treatment plans they’re bought into.
At CooperRiis, we are not interested in subduing anyone into social conformity. Instead, we aim to support residents in managing their symptoms so they can express themselves as fully and authentically as possible. That’s why we’re more than an inpatient bipolar treatment facility; we’re a whole-person recovery center.
Collaborating To Recover
Consistency and self-care are critical for staving off manic or hypomanic and depressive episodes. We collaborate with residents to establish medication protocols and social rhythms that will help them maintain their emotional equilibrium after their time at CooperRiis. We also help them recognize early signs of symptom development and adopt effective coping strategies, enabling them to interrupt spirals on their own.
By helping residents cultivate lifestyles and acquire symptom management skills that are tailored to their unique needs, preferences and goals, we ensure the self-regulation strategies they learn within CooperRiis are transferable outside of it. In this way, our program does more than temporarily mitigate symptoms; it lays the foundation for lifelong wellbeing.
Strong Support Networks
Integrated, Whole-Person Treatment
Individuals with bipolar disorder respond best to multimodal treatment plans that combine medication with sustainable lifestyle interventions. That’s why, rather than relying exclusively on any one type of treatment, we combine a variety of evidence-based therapies to address all of the following seven domains of health for our residents:The Seven Domains of Recovery
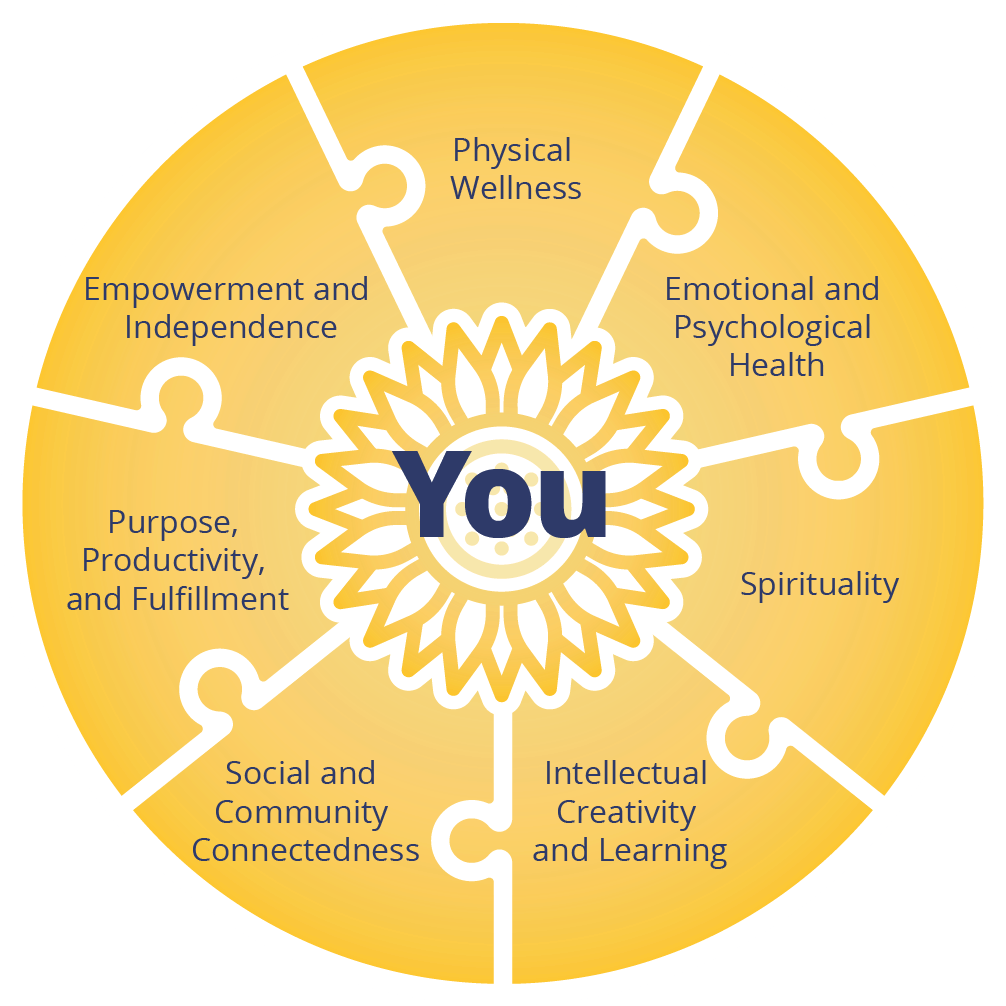
Treatment Plans That Meet Residents Where They Are
Consistent, Soothing Environment
WRAP Groups
Exercise/Movement Practices
Nutrition and Supplements
Medication
Self Care Routines
Psychotherapy
Community
Family Education
Our Recovery Model Works
Data collected over 10 years show that the residential treatment program for bipolar disorders at CooperRiis works. Individuals who benefit from our holistic, recovery-focused model of care make demonstrable progress in multiple domains of health.
After participating in our program, people with bipolar disorder:
- Experience improved emotional stability.
- Are better able to maintain work, relationships, and personal health.
- Possess a more unified, positive sense of self.
- Are empowered to become stewards of their own health.
An extensive body of research and clinical experience affirms these findings: Combining psychotherapy with a strong, supportive community, structured daily routines, physical wellness programs, and an integrative approach to medication can dramatically improve the lives of individuals with bipolar disorder.
2019 Alumni Survey Results
are engaged in either competitive employment, volunteering, or going to school.
Research Citations
1Pelletier, L., Shamila, S., Scott B., P., & Demers, A. (2017). Self-management of mood and/or anxiety disorders through physical activity/exercise. Health Promotion and Chronic Disease Prevention in Canada: Research, Policy and Practice, 37(5), 27–32. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5650020/
2Tomita, A., Lukens, E. P., & Herman, D. B. (2014). Mediation analysis of critical time intervention for persons living with serious mental illnesses: Assessing the role of family relations in reducing psychiatric rehospitalization. Psychiatric Rehabilitation Journal, 37(1), 4–10. https://doi.org/10.1037/prj0000015