Just under 3% of Americans have some form of bipolar disorder. If that includes you or someone you love, there is good and bad news.
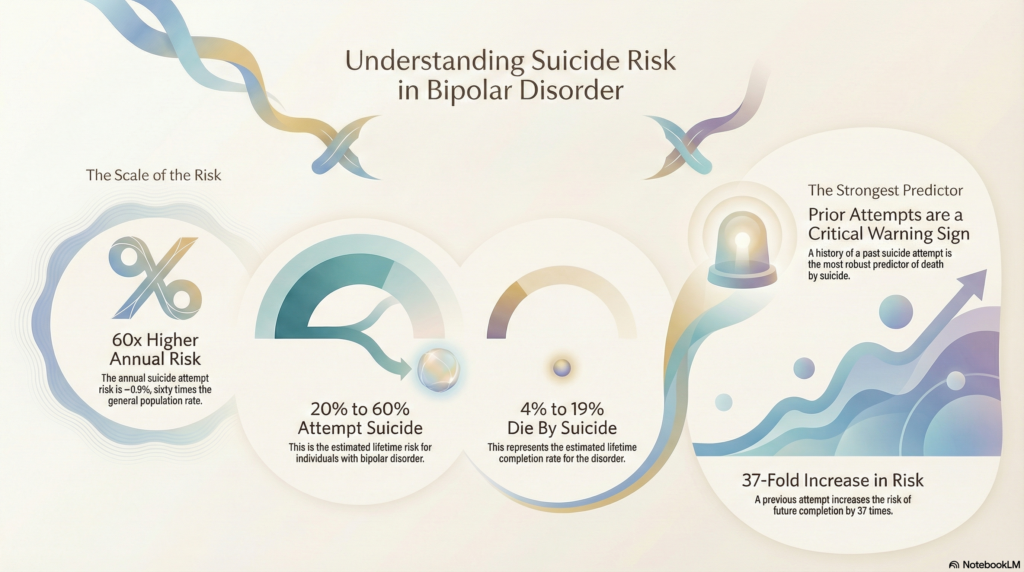
First the bad news: Bipolar disorder comes with a 64% excess mortality rate. As many as one in five people with bipolar ultimately dies by suicide, and this population’s risk of suicide death is ~60 times higher than that of the general population.
Now, the good news: This doesn’t have to be you or your loved one. Those numbers speak to the public health picture, and bipolar disorder is treatable. At the individual level, suicide risk can be reduced by 80% or more. Let’s take a deeper look.
What is Bipolar Disorder?
Bipolar disorder describes a family of mental health diagnoses, which includes Bipolar I, Bipolar II, Cyclothymic Disorder, and other subthreshold variations. It is characterized by recurrent mood episodes, including mania or hypomania and depression. Many with a bipolar condition also experience circadian differences.
A note about diagnoses: At CooperRiis, we believe a person is profoundly more than their diagnosis. As such, within our residential programs, we don’t place emphasis on diagnosis in daily life. While it’s carefully considered from a clinical perspective, this is between the individual and their therapist. We do, however, believe deeply in providing much-needed diagnosis-specific education to individuals and families.
What Are the Risk Factors for Suicide in Bipolar Disorder?
Each person who lives with bipolar disorder has their own individual level of risk, depending upon many modifying factors, some that we can name and others which remain unknown. And, while these factors are meaningful at the population level, individual risk factors for suicide vary significantly.
Furthermore, for as alarmingly at-risk as the bipolar population is, [statistical] suicide risk moderation is woefully understudied. Researchers have, however, identified several modifying risk factors for suicide with reasonable certainty:
- Sex: men are more likely to die by suicide, but women are more likely to attempt it.
- Age: under 35 or over 75.
- Marital status: single, divorced, or widowed.
- Employment: being under- or unemployed.
- Family status: single parent or childless.
- Clinical history: prior attempt, family history of suicide.
- Psychological comorbidities: Cluster B personality disorder, substance use, eating disorder, anxiety disorder, ADHD.
- Bipolar characteristics: earlier-age onset, longer time untreated, presence of psychosis, depressive-predominant or rapid cycling polarity.
- Institutional encounters: criminal convictions, previous involuntary confinement.
- Trauma: history of childhood abuse or neglect.
- Current circumstances: recent bereavement, interpersonal problems, financial or occupational crisis, sleep deprivation.
- And, curiously: Living at higher altitude.
What Reduces Risk of Suicide in Bipolar Disorder?
While the risk of suicide in bipolar disorder and the statistics around it are scary, bipolar is one of the most treatable serious psychological disorders. Integrative treatment, including medication, regular therapy, and psychoeducation can bring some people’s individual risk to near zero. The following are the four greatest protective factors:
Lithium
By far the most-studied, best-founded risk-reducing modifier is a mood-stabilizing drug known as lithium. Research has found that its prescription form can reduce risk of suicide in bipolar patients by 60 to 80%. Other mood-stabilizers may have similar protective effects, but the long-term data does not yet exist for them.
Social and Family Bonds
Some of the most protective networks in the lives of those with bipolar disorder are immediate family and supportive community relationships. Simply living with others appears to offer a 60% reduction in suicide risk, but clinical evidence suggests being married (or cohabitating) with children offers the strongest buffer. Outside of the home, all social connection improves prognosis: close friends, faith groups, work or volunteer communities, even passing acquaintances like baristas and gym regulars have some positive impact.
Religious or Moral Beliefs
Anyone with a strong spiritual or moral objection to suicide is less likely to attempt it. One study found that religious affiliation correlated to a 21.5% reduced risk of suicidal behavior.
Consistent Mental Health Care
Having seen a mental health professional within the past week is correlated with a much lower risk of death by suicide in bipolar disorder—64%, according to one literature review.
When is Suicide Risk Highest in Bipolar Disorder?
You might wonder why—if bipolar is so treatable—are the statistics around suicide still so grim? The answer to this question lies at least partly in when the highest risk occurs. High-risk times fall into two main categories: treatment transitions and episode types.
- Treatment transitions: stopping or losing access to treatment, including hospitalization, therapy, or medication; changing medications; going from inpatient to outpatient care; awaiting diagnosis.
- Episode types: depressive, major depressive, and mixed depressive episodes. Transitions between episode types may represent additional risk.
Often, people resist or do not receive the extra support they need during these times of transition, which can be catastrophic.
How Can You Reduce Individual Risk?
Putting together what we’ve learned about the risk-enhancing factors, risk-reducing factors, and high-risk windows, we can surmise a few high-leverage protective actions. Some items are certainly more actionable than others. It’s much easier to make a therapy appointment than to get married and have children, for example, but each protective factor offers something:
Consider Medication
While medication is not right for everyone, it can make a life-and-death difference for many. It is likely the single biggest lever.
Live Socially
If you’re married with children, great—you’ve got a built-in protection. If not, living with others, like roommates, family members, or chosen family still offers an important buffer. And, simply being involved in community not only protects against death by suicide; it also offers partial protection against depressive episodes.
Spiritual Engagement
While most people can’t simply adopt a religious or moral belief set on command, it can still be helpful for some people with bipolar disorder to lean into any religious or spiritual beliefs they already have. There may be a subset for whom this is not healthy, but the single study that points to this finds correlation, not causation, and under very specific circumstances.
Mental Health Care
See a therapist or psychologist every week; don’t stop. If depression starts to creep in, resist the urge to cancel. Consider adding more weekly sessions or stepping up to a higher level of care instead. During transitions, seek all the support available. For example:
- Multiple therapy sessions per week during medication or dose changes.
- Residential or partial hospitalization (PHP) after inpatient care.
- Transitional housing or PHP after residential care.
- Work closely with a psychiatrist if stopping meds, and explicitly follow their guidance.
- Immediately seek community-based mental health options if insurance stops or access to care is otherwise interrupted.
- In the case of delayed or misdiagnosis, do not wait for answers before seeking help. Mental health professionals don’t need a diagnosis to be there for you.
Support Resources & Suicide Prevention
It may feel unsafe to talk with healthcare providers, or perhaps burdening to share with loved ones, about suicidality; but other resources are available to prevent this from creating or prolonging isolation. If you or someone you love is thinking about suicide, you can call or text 988 Suicide & Crisis Lifeline to reach trained counselors 24/7, or use chat at 988lifeline.org.
If you’re not in immediate crisis but want to talk with someone who understands, 7 Cups offers free, confidential emotional support through trained listeners, as well as optional therapy resources. This alone can provide life-saving space and perspective.
If you are (or someone else is) in immediate danger, call 911 (or your local emergency number). If you’re outside the U.S., you can find international crisis resources at findahelpline.com. All of these resources are also available to anyone who may need guidance with helping or protecting someone they care about.
Residential Care Offers Several Protections Against Suicide in Bipolar Disorder
CooperRiis is a residential mental health community offering short- and longer-term bipolar treatment programs centered around recovery-focused care. This means that we don’t exist simply to help folks survive bipolar disorder. We’re here to help you build a stable and fulfilling life.
By offering simultaneous access to all of the protective factors covered here and more, we support residents as they stabilize, set goals, gain self-understanding, develop coping tools, improve physical health, and build a more at-peace sense of self. Through living and healing in community, purposeful daily work, rigorous clinical care, and the time and space to access their own spiritual truths, residents leave CooperRiis with tools to thrive.
Please feel free to explore our programs or contact admissions if this feels like the level of care that you or your loved one needs.